|
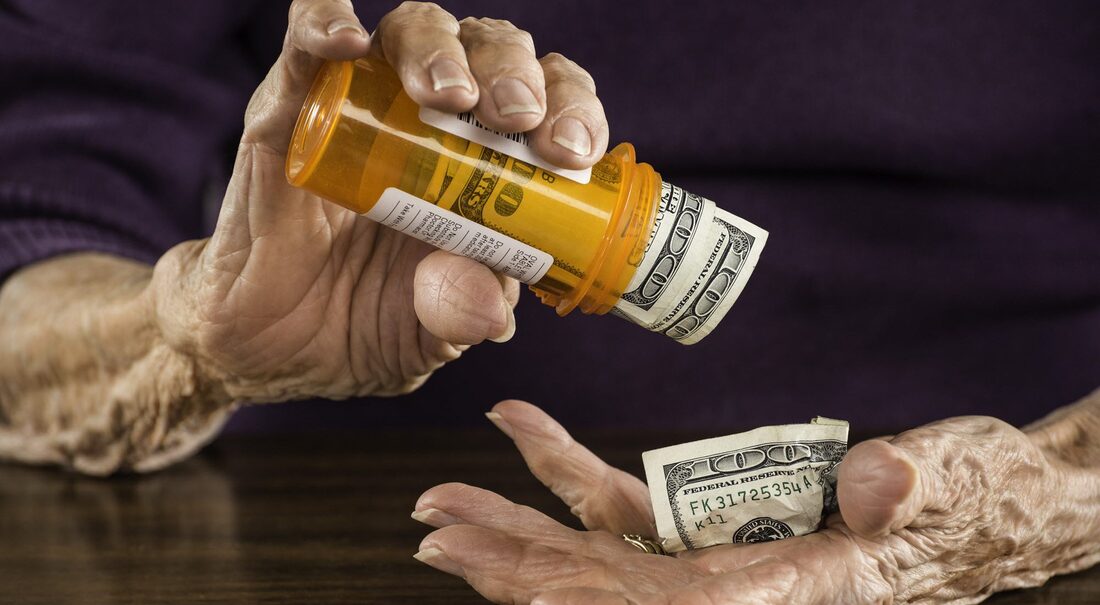
Did you or someone you work with fall into the Medicare Part D “donut hole” this year?
The donut hole, or Part D coverage gap, occurs when a person reaches a certain spending limit for their medications ($3,820 in 2018), and must pay more of the costs after crossing that threshold. Here’s how you can try to avoid the donut hole altogether and get financial assistance if you do fall into the coverage gap. The importance of shopping aroundThe Annual Enrollment Period for Medicare Advantage and Part D plans runs October 15 – December 7. During this time, people with Medicare can join, switch, or leave plans. This Part D plan checklist, developed for NCOA by the Medicare Rights Center, provides a list of questions to ask before selecting prescription drug coverage. Aside from looking at costs, you also want to make sure that you choose a plan that covers all/most of your medications and makes it convenient for you to obtain them. Using the Medicare Plan Finder, you can enter your prescription information and compare plans to determine what your costs may be in the coming year, including when/if you would expect to fall into the donut hole. Some plans may offer additional coverage during the coverage gap, like for generic drugs; however, they may charge a higher monthly premium. Working with an unbiased counselor, such as those at your State Health Insurance Assistance Program (SHIP) can help. Or use the questionnaire at NCOA’s My Medicare Matters to get recommendations about your coverage options. Isn’t the donut hole closing in 2019? You may have heard that the Affordable Care Act set in motion plans to close the Part D coverage gap by 2020, which was advanced a year in recent Medicare legislation. But “closing” does not mean that people reaching the donut hole do not pay anything for their drugs—it means that plans and pharmaceutical companies pick up more of the tab. Beginning in 2019, Medicare beneficiaries enrolled in Part D prescription drug plans reaching the donut hole will still pay 37% of the costs of their generic medications, and 25% of the brand-name medications. Getting help in the gapIf you cannot avoid the donut hole, you’ll want to explore these options to help pay for your prescriptions:
You can use NCOA’s free, comprehensive screening tool Benefits CheckUp to see if you qualify for any of these and other money-saving benefits. Avoiding the coverage gap entirely If you have limited income and resources, you may want to see if you qualify to receive Medicare’s Extra Help/Part D Low-Income Subsidy. People with Extra Help see significant savings on their drug plans and medications at the pharmacy, and do not fall into the donut hole. No matter which off exchange health insurance you choose, the prices of health insurance will always be the same.
1 Comment
A new opportunity to switch Medicare Advantage/Part C plans is happening right now. The annual Medicare Advantage Open Enrollment Period (MA OEP) which runs from January 1 to March 31 offers anyone enrolled in a Medicare Advantage plan an opportunity to either:
Think of the Medicare Advantage Open Enrollment Period as an exchange period. Typically, when you enroll in a Part C plan during the Annual Election Period (October 15 – December 7) you have to keep the plan for the entire year until the next election period. However, with the MA OEP if you enroll in a plan that doesn’t fit your needs you can switch immediately after your new plan becomes effective on January 1. Once you select a new Part C or Original Medicare plan, your new plan becomes effective the month after your switch. You are only allowed to switch once time during the annual MA OEP. You may ask, “why go through the trouble of searching for another Medicare Advantage plan again?” and the answer varies depending on your situation. You may have enrolled in a Medicare Part C plan in October, started using it at the beginning of the year and realized that the doctor you want to see is not in-network, or your out-of-pocket costs were higher than expected. Maybe you want freedoms not offered by MA plans like visiting any Medicare-approved doctor regardless of networks. Whatever the reason, you now have an opportunity to do so without facing any penalties. If you decide to switch to Original Medicare and enroll in a Medigap plan check with your State Health Insurance Assistance Program for Medigap enrollment information. Two Opportunities The Medicare Advantage Open Enrollment Period consists of two separate periods in which you can switch plans. The previously discussed period was the annual Medicare Advantage Open Enrollment Period (MA OEP) which runs from January 1 to March 31. There’s also an individual Medicare Advantage Open Enrollment Period that varies depending on when you first enroll in Medicare. The difference between the two periods is this:
Both periods offer the same enrollment options, either switch from one Part C plan to another, or switch from a Part C plan to Original Medicare and add Part D prescription drug coverage. The only difference is when you’re allowed to do so. How to use the MA OEP Similar to other enrollment periods, to start searching for a new Medicare Advantage plan we recommend you start by taking our Medicare Questionnaire, created by the nonprofit National Council on Aging. You’ll get free Medicare advice from a licensed Medicare benefits adviser or local State Health Insurance Assistance Program (SHIP) to help you figure out your options and choose a new plan. Before you speak with a healthcare exchange pa expert figure out what questions you should ask to find the best coverage for your needs. Getting the best price: how filling a prescription is like filling your gas tank.You’re running low on gas, and there are two gas stations nearby. Do you stop at the closest one? The one with the best coffee? Or the one advertising the lowest price? If you’re like me, lowest price usually wins.
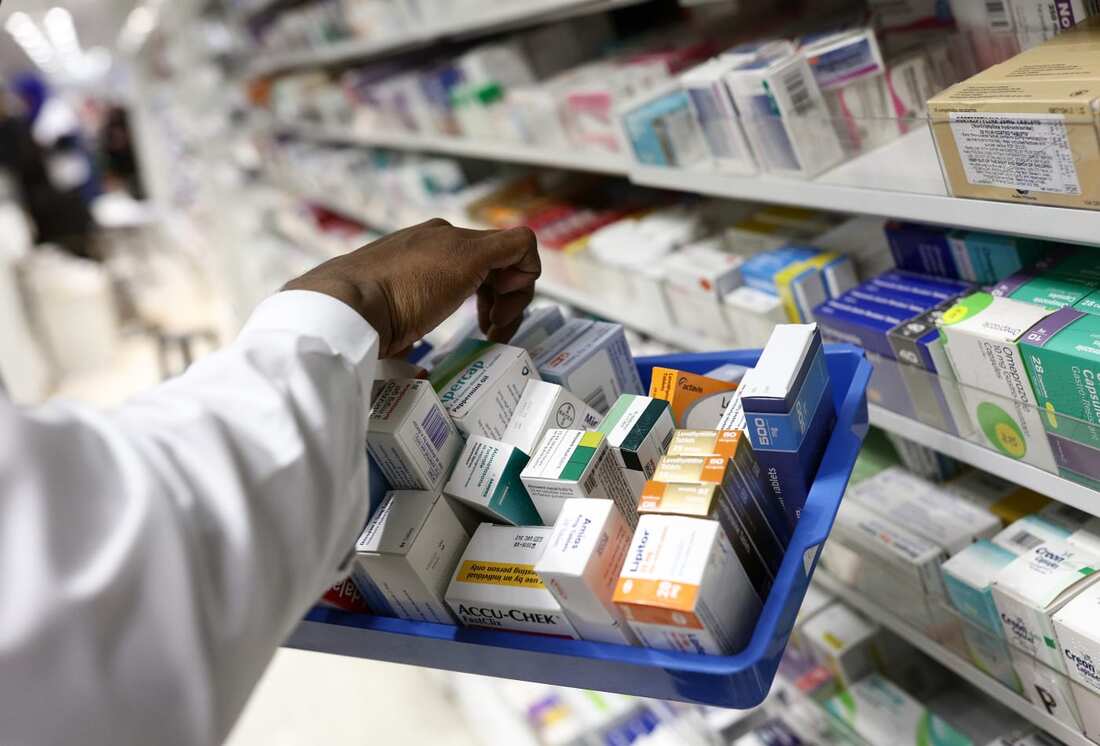
Getting a prescription filled is a lot like filling your gas tank. Did you know that prices vary from pharmacy to pharmacy for the same medicine? And, these prices can change often. Also, similar to the gas stations, the larger, well-known pharmacy chains don’t necessarily have the most competitive prices. Just like gas stations, pharmacies can set their own prices for medicines. They just have to stay within a certain range determined by the type of medicine it is and agreements they have with your particular health insurance plan. Manufacturing shortages and supply issues can also affect medicine prices – just like oil prices. The bottom line? If you’re spending a lot of money to fill regular prescriptions, it pays to find the best deal. 2 ways to shop for the best prescription cost with Medicare Unlike gas stations, pharmacies don’t post their prescription prices on brightly lit signs out front. But there are still ways to find out how much your medicine will cost before you make the trip.
5 ways to lower your medicine costsSometimes, like in the case of a medicine shortage, it’s just not possible to get a better deal. That’s when you could talk to your doctor about making a change. Here’s what you can ask your doctor about: 1. Instead of ordering enough for 90 days, can you order a 30-day supply? The price of the medicine might go down in a month or two. Then you can go back to purchasing a larger supply. However, don’t skip months or days to save money. 2. Is there a different version of the same medicine? For example, if you’re taking an extended-release version of a medicine once a day, you could try a less expensive, immediate-release version twice a day instead. The cost savings might make up for the inconvenience of taking two doses. 3. Is there a generic or preferred version of the same medicine? By law, generic versions of a medicine must use the same active ingredients and meet the same quality and safety standards as the brand name medicine. Generics are typically less expensive. 4. Is there someone who can help me look at all of my medicines? If you’re taking more than one medication regularly, consider scheduling a visit with a Medication Therapy Management (MTM) Pharmacist. These clinical pharmacists work closely with your doctor to look at your medicines, separately and together, to see how your medicines interact with each other. They can suggest less expensive versions of the medicines you’re taking and work with your doctor to see if you might be ready for a lower dosage. 5. If you have sticker shock at your pharmacy counter, let the pharmacist know that you need to get more information about the cost. Then, call your health insurance company. They’ll be able to help answer your questions and let you know if there are less-expensive options available to you. You or your pharmacist can also work with your doctor to find other off exchange health insurance options. You wake up on Jan. 1 to a new year, full of new possibilities and with it, a new amount you have to pay for your medicines before your health or drug plan helps. This is called your deductible. Your deductible resets at the beginning of each year and is the amount you’ll need to pay before your insurance kicks in.
Read on for tips about how to prepare when you are at the pharmacy counter and unexpectedly have to pay full price for your medicines. Try these tips to avoid sticker shock
Prepare now for next year’s resetThe good thing is now you know your deductible resets each year. Planning for your medicine costs to be higher at the beginning of the year can help you budget.
“Is this covered?” It’s one of the most common questions I get from members wondering about seeing a new doctor, changing medicines or trying a new treatment option. And I’m glad they call and ask me. Knowing what appointments, tests, screenings and other services your Medicare plan coverage pays for is the first step to understanding how much you’ll have to pay for your health care.
What “covered” meansIf something is “covered,” it means your Medicare plan will help you pay for it. How much the plan pays depends on the type of care you use and where you get it. To get the most cost effective health care, you’ll want all the services you use to be covered by your Medicare plan.
Checking what’s covered Keep these areas in mind when checking coverage for each plan: DoctorsMedicare plans cover specific doctors, specialists and clinics, often referred to as a network. There are ways to find quality doctors who also offer the most coverage when you see them.
Medicines Plans have a list of medicines, called a formulary, which shows what medicines they cover. The list can give you a general idea of what you may pay for your medicines.
Different medicines are covered differently. For example, generic medicines are usually less expensive than brand-name medicines. So ask how much you’ll have to pay, and make sure it fits your budget. If it’s too expensive, your doctor can help you find a different drug, or the pharmacy might have a rewards or payment program. Services From doctor visits and physical therapy sessions to blood tests, X-rays, ambulance rides and hospital stays, Medicare plans cover health care services differently.
Healthcare exchange pa plans should only be considered by people who are in good health and who do not frequently use medical services. If you want to know more details please contact us. We’re living in the digitally connected 21st century! There is more information about Medicare online than ever before. So where do you start? How do you weed through it all when you’re researching and shopping for a plan?
The Medicare Plan FinderI talk to members all the time who want to know the best online tools to search for and sign up for a Medicare plan. Right away, I tell them to check out the Medicare Plan Finder. The Medicare Plan Finder allows you to really compare your health plan options. It’s a good place to start your research. Unlike the private Medicare plan sites, Medicare.gov looks at everything across all Medicare plans. You’ll be able to see and compare how Medicare plans stack up against each other. Once you find a plan that suits your needs or at least piques your interest, use the private health plan sites to get more details. Dig deeper to check benefit levels – a benefit level is the maximum amount a health insurance company agrees to pay for a specific covered benefit. And learn more about plan offerings and any extras that may be included such as fitness benefits or discounts. Does my doctor accept my Medicare plan?If it’s important to you to keep your favorite doctors, visit Physician Compare to find your provider. And when it comes to private plans, you’ll want to see what doctors are covered by the insurance plans you’re interested in. Providers who accept Medicare may be listed as “Medicare certified” or “accepting Medicare assignment.” Be safe and secureTake the same online precautions you would when you’re shopping for anything else online. Never sign anything or give out your personal information unless you’re sure you’re on a secure web site. Doing your Medicare research has never been easier – you can learn a lot online about your Medicare options. What’s most important is that you know what you’re shopping and signing up for, and that you get the plan that best fits your wants and needs. Off exchange health insurance plans offer the same sorts of coverage that are available with ACA plans. If you want to know more details please visit us. Since I live in the Midwest, where “polar vortex” is actually a thing, I’ve always dreamed of spending the winters somewhere warm. I know a lot of Medicare members are in the same boat. Maybe you want to get away to the beach or the golf course, or just be closer to your grandkids. Wherever you want to go, it’s important to know if your health care needs are covered.
What is a Medicare Advantage travel benefit?A lot of people choose to get their Medicare benefits through a Medicare Advantage plan. One of the benefits of this kind of plan is that you can save money on health care costs if you see doctors, clinics and hospitals that have agreed to provide plan members with health care services (called a network). If you’re spending part of the year away from home, here are a few things to keep in mind:
With a travel benefit, you’ll pay almost the same for care out-of-state as you would close to home. The benefits and costs are different for every plan, so you’ll need to do your homework to figure out what’s best for you. How does a travel benefit work? Some travel benefits, such as those for international travel, are based on where you’re going. Others cover you for a certain time period — say December through April at your home-away-from-home. So a benefit like this might get you the same services for roughly the same out-of-pocket costs you’d pay at home. It’s pretty common for your health plan to require that you be away from home for a few weeks or months before the benefit kicks in. That’s because perks like this are meant to cover longer stays instead of short vacations. And like we talked about, you’re always covered at network rates when you have an emergency while traveling. Not all Medicare Advantage plans include a travel benefit. So if you’re like me and plan on traveling south every winter, you should look for a plan that offers one. Some are included in the price of your plan. Others are an option that you pay for only when you need it. Because every plan is different, contact your plan to learn more. Off exchange health insurance plans are purchased without going through the ACA exchange in your state. They can be purchased directly from an insurance company, or with the help of a broker. If you’re joining the ranks of workers 65+, Medicare might be the last thing on your mind. But when 65 is just around the corner, there are some important things you should know.
Four common Medicare questions 1. Can I delay signing up for Medicare Part B? If you have medical coverage through an employer, or you’re covered under your spouse’s employer plan, you can delay enrolling in Medicare Part B, which covers medical services, without paying a penalty. Many people don’t enroll in Medicare Part B until they stop working. Once you’re not covered under your employer plan (or your spouse’s), you’ll have eight months to enroll in Medicare Part B without paying a penalty. 2. How does enrolling in Medicare affect my HSA plan? If you have a health plan through your employer and it includes a health savings account (HSA), signing up for Medicare Part B, or being enrolled in Medicare Part A, will change things. You can stay on your employer plan, but you can’t add money to your HSA once you enroll in Medicare. If you’re considering this option, it’s a good idea to check with a financial adviser. They know the ins and outs of how Medicare will affect your HSA and your taxes, and can help you figure out your best option. 3. When should I start planning for retirement? Choosing a Medicare plan can be a long process! There’s a lot to consider and it takes time to find the right plan for you. If possible, I recommend starting your search about six to nine months before your retirement date. This gives you enough time to look into the plans that interest you. If you don’t have that much time, call plan advisers at private insurance companies that you’re interested in, or meet with someone who sells plans from multiple insurance companies (called a broker or agent) one-on-one. They can help you quickly find a plan that fits your needs and budget. 4. How will my current employer plan work with Medicare? If you have Medicare and also have health insurance through your job, these plans will work together. The coverage through your job will pay for some services, and your Medicare plan might cover some other services. If you have questions about off exchange health insurance plans, ask for advice from your current plan or benefits office. When I first started my career in the Medicare world, I was overwhelmed with all the new information I had to learn. I found that breaking it down into bite-sized pieces made it easier to understand. It took a lot of time (and patience), and one of the hardest parts was understanding all the different parts of Medicare. Here are some tips that helped me understand Medicare.
What is Medicare?Medicare is a federal health insurance program for people 65 and older, people under 65 with certain disabilities and people of all ages with end-stage renal disease. Medicare is partly funded by payroll taxes from most employers, employees and all people who are self-employed. The Medicare program offers basic coverage to help pay for things like doctor visits, hospital stays and surgeries. What are the parts of Medicare?Medicare is broken out into four parts.
Medicare Parts A and BParts A and B are known as Original Medicare. This is the most basic coverage you can get. Medicare Parts C and DParts C and D are available through private health plans. They’re both ways to enhance your health care coverage if you want more than what Original Medicare offers. Medicare Parts A, B, C and D explained:
When can I get Medicare? You’re eligible for Medicare when you turn 65. There are a few different times you can enroll throughout the year. These are known as enrollment periods. Check out the off exchange health insurance, or visit us for more information. October is National Ergonomics Month, and there’s no better time to evaluate your office environment. You may think that crafting an ergonomic workspace is mostly about getting certain chairs or keyboards, but in reality the principles of this field go far beyond comfort.
Making an office more ergonomic leads to healthier, more productive employees. Here’s how. What Is an Ergonomic Space?Ergonomics explores how people can work better and more efficiently. In general, an ergonomic workplace uses information about how people work to make changes that promote and protect employees’ health. This is critical for jobs with repetitive tasks like lifting, jobs involving many tools or jobs with long bouts of sitting and typing. When employees work in an environment that doesn’t make sense for them, they risk spending long periods of time in awkward positions or performing tasks that put them at a higher risk of developing musculoskeletal disorders (MSDs). And those injuries pose a big problem for the workforce. MSDs include injuries such as:
The Occupational Safety and Health Administration reports that 33% of worker illnesses and injury cases were due to MSDs. They’re also the leading cause of lost working days and reduced work. Ergonomics in the workplace may be even more important for aging Baby Boomers who are waiting longer to retire. For instance, sitting for long periods and with poor posture can lead to lower back pain. It’s a condition that affects all age groups, but people over 55 experience it more frequently. About 47% of workers older than 55 have arthritis, while 44% have hypertension, and they are the most likely age group to develop carpal tunnel syndrome. An office environment that doesn’t fit their needs can exacerbate these issues. How to Improve Ergonomics in the WorkplaceCreating an ergonomic environment starts with assessing your current situation. Consider the tasks your employees do in a typical day: Walk around desks, through a warehouse or along an assembly line to observe the repetitive movements employees perform. Note where you observe poor posture, strenuous lifting requirements or heavily used tools, and look for opportunities to make the employees more comfortable and less prone to injury. Make special note of any adjustments employees have made to their space or items themselves, such as placing cushions on desk chairs; they may indicate that your employees already know where there’s room for improvement. Once you have a list of possible hazards in hand, consider following the guide to implementing an ergonomics program in the workplace created by the Centers for Disease Control and Prevention. The guide recommends a hierarchy for making changes, starting with eliminating risks that could cause falls, slips or injuries. You can also change the way people work and ensure they have equipment that lessens MSDs, such as adjusting chairs and monitors to the appropriate height for good posture or introducing assisted devices for lifting and moving products through a warehouse. If you’d prefer having a professional make the assessment, ergonomics experts can come to your office to perform an analysis and make recommendations. However, just making a few small changes with your workforce’s needs in mind is enough to make a difference and keep your employees working in style — and, more importantly, in comfort. Do you want to know more details about health insurance please visit our service area. WASHINGTON — Senator Elizabeth Warren vowed on Friday to pass major health care legislation in her first 100 days as president, unveiling a new, detailed plan to significantly expand public health insurance coverage as a first step, and promising to pass a “Medicare for all” system by the end of her third year in office that would cover all Americans.
The initial bill she would seek to pass if elected would be a step short of the broader Medicare for all plan she has championed. But it would substantially expand the reach and generosity of public health insurance, creating a government plan that would offer free coverage to all American children and people earning less than double the federal poverty rate, or about $50,000 for a family of four, and that could be purchased by other Americans who want it. Ms. Warren has long endorsed a Medicare for all bill sponsored by one of her rivals for the Democratic nomination, Senator Bernie Sanders of Vermont. But until now, she has not specified how quickly she would move to enact a health care plan. Friday’s proposal amounts to a detailed road map for eventually establishing Medicare for all, a single government-run health insurance program under which private coverage would be eliminated. That goal — a wholesale transformation of how Americans receive health insurance — is a big political gamble, particularly given that many of them would have to give up the coverage they get through their employers. Ms. Warren’s proposal for Medicare for all would require an estimated $20.5 trillion in new federal spending over a decade, according to a financing plan she released two weeks ago. To provide funding for it, she would impose new taxes on businesses and the richest Americans. But under the plan she presented on Friday, she would not seek passage of a single-payer system early in her presidency. The proposal would instead move people into that system gradually — in a way she hopes would build public support for full-fledged Medicare for all — while temporarily preserving the employer-based insurance system that covers most working-age adults today. “I believe the next president must do everything she can within one presidential term to complete the transition to Medicare for all,” Ms. Warren, of Massachusetts, wrote in her plan. “My plan will reduce the financial and political power of the insurance companies — as well as their ability to frighten the American people — by implementing reforms immediately and demonstrating at each phase that true Medicare for all coverage is better than their private options. I believe this approach gives us our best chance to succeed.” Though the details differ, Ms. Warren’s transition plan shares many features with health care proposals from her more moderate rivals for the nomination, including Joseph R. Biden Jr., the former vice president, and Pete Buttigieg, the mayor of South Bend, Ind. For example, it would allow higher-income adults to voluntarily sign up for a new public plan. Ms. Warren’s proposal, however, would make the optional government plan more generous than those proposed by her rivals, and would allow more Americans to get it free. It would also let anyone over 50 buy Medicare coverage, with more benefits than the program offers now. With her interim plan, Ms. Warren is attempting to offer something attractive to both sides of the Democratic health care debate: preserving her commitment to the single-payer vision that energizes voters on the left, while offering a less disruptive set of proposals in the short term to those who may be reluctant to give up their existing coverage. But her choice to put off seeking passage of a full-scale Medicare for all plan until as late as her third year in office could draw criticism from liberals eager to put in place a single-payer system as quickly as possible. “Now, some people say we should delay that fight for a few more years,” Mr. Sanders said on Friday as he discussed Medicare for all and the opponents who would try to stop it. “I don’t think so. We’re ready to take them on right now, and we’re going to take them on on Day 1.” And on Twitter, he offered his own pledge about the beginning of his presidency: “In my first week as president, we will introduce Medicare for All legislation.” Representative Pramila Jayapal, Democrat of Washington, who has introduced Medicare for all legislation in the House, praised Ms. Warren’s plan as “one smart approach” that “gets us to Medicare for all that covers everyone with comprehensive care in four years.” Ms. Warren’s plan reflects a sense of pragmatism about the politics and logistics of passing a major health bill through a closely divided Congress. Ms. Warren said she would pass the transition plan using special procedures that would require only a simple majority in the Senate, rather than the 60 votes needed to overcome a filibuster. But she would still rely on Democrats winning control of the Senate, where Republicans currently hold a slim majority. And she is laying out ambitious details for getting to a single-payer system even as voter support for the idea is narrowing; polls suggest substantially more Americans prefer the “public option” type of plans that Mr. Biden and Mr. Buttigieg have proposed. Kate Bedingfield, a deputy campaign manager for Mr. Biden, said Ms. Warren was “trying to muddy the waters even further” after “having discovered how problematic her embrace of Medicare for all has become.” “What started out as ‘mathematical gymnastics’ have been replaced by a full program of flips and twists covering every element of her plan,” she said, adding that the transition plan “doesn’t change the reality that Medicare for all will deny Americans the right to choose their insurance by eliminating employer-sponsored insurance.” Passing a health bill could crowd out other legislative priorities. President Trump’s efforts to repeal and replace major parts of the Affordable Care Act in 2017 stretched well beyond his first 100 days and ultimately failed. And given the unpredictable nature of politics, a pledge to pass comprehensive Medicare for all legislation by the end of 2023 represents a somewhat distant goal. “I think that it’s really unnecessary and potentially dangerous to try to split up something like Medicare for all into multiple bills,” said Dr. Adam Gaffney, the president of Physicians for a National Health Program, a group of doctors that supports a single-payer health care system. But he said he was pleased Ms. Warren was still advocating Medicare for all. When Ms. Warren laid out her plan to finance a Medicare for all system earlier this month, she said that she would not increase taxes on middle-class families by “one penny.” Among other revenue sources, Ms. Warren would require employers to pay an amount similar to what they are currently spending on their employees’ health care, and she would raise taxes on the richest Americans, including by steepening her proposed wealth tax for billionaires. Her transition plan did not come with its own detailed financing proposal, but it said the interim program would cost the federal government less than an eventual Medicare for all system and would be funded using some mix of the revenue sources she has already identified. The plan also spells out a long list of administrative actions Ms. Warren would take to change the health care system, even if Democrats do not retake the Senate. She would roll back Trump administration regulations that have weakened the Affordable Care Act and broaden benefits in the existing Medicare program. She would also use executive authority to allow new generic versions of expensive drugs — such as insulins taken by patients with diabetes, treatments for hepatitis C and the overdose reversal drug Naloxone — in an effort to lower their prices. As Ms. Warren has established herself as a leading candidate for the Democratic nomination, her opponents have frequently attacked her over health care, a top issue in the primary. For much of the fall, her refusal to say whether she would raise taxes on the middle class provided an opening for some of her rivals to paint her as cagey on a key issue. Mr. Biden and Mr. Buttigieg have also argued their public option proposals are far more realistic than Ms. Warren’s plan for Medicare for all, emphasizing that her plan would take away people’s private health coverage. Lis Smith, a senior adviser for Mr. Buttigieg’s campaign, described Ms. Warren’s transition plan as “a transparently political attempt to paper over a very serious policy problem, which is that she wants to force 150 million people off their private insurance — whether they like it or not.” In the longer term, Ms. Warren’s embrace of Medicare for all would provide ammunition to Mr. Trump and his Republican allies if she became the Democratic nominee. Mr. Trump is already fond of equating Democratic approaches to health care with socialism. Ms. Warren is a co-sponsor of Mr. Sanders’s Medicare for all legislation, which includes a four-year transition. Though his legislation is best known for its endpoint, it includes a detailed plan for moving from the current health care system to that final goal. But Mr. Sanders’s transition relies on passing his entire plan. Ms. Warren, by contrast, has suggested splitting the process in two: starting with the transition plan and only later passing a full Medicare for all bill. And Mr. Sanders, unlike Ms. Warren, has declined to specify a detailed financing plan for his proposal. Do you want to know more details about health insurance please visit our service area. The Democratic presidential candidates have been fighting over whether they should try to replace the health insurance system with a single government-run plan or create a government-run plan that Americans could choose to join.
But hidden outside this big debate is a harsh reality: If Democrats fail to retake control of the Senate, neither plan has much of a chance to become law. Elizabeth Warren, the Massachusetts senator, has allied herself with the “Medicare for all” wing of the party, saying she would propose a single-payer system. But on Friday, she released a second plan, a sort of steppingstone along the way that would create a more optional government program. Her transition plan is engineered to pass with only a majority of Senate votes, instead of the 60 usually needed to overcome a filibuster. But it also includes a long and detailed list of the things she would do if she couldn’t get Congress on board. That section of the report, which is likely to get less attention and draw less criticism than the rest, actually tells us a lot about what health care policy would probably be like in a Warren administration. President Trump was elected in part on a promise to transform the health care system. His efforts to repeal and replace the Affordable Care Act have been unsuccessful, as Republicans in the Senate are unable to agree on any one solution. But he has used his regulatory authority to make many of the changes he was unable to achieve through Congress, like expanding the availability of insurance plans that cover fewer benefits; reducing federal funding of Planned Parenthood; permitting states to establish work requirements for Medicaid benefits; and increasing the size of special accounts that workers can use to save money for health care expenses. He has also pursued other regulatory projects in health care, like his proposal, finalized on Friday, that would require hospitals to publicize the prices they have negotiated with insurance companies. He is allowing states to import drugs from Canada through regulatory power, and aiming to overhaul care for patients with renal disease. So what would Warren do? Her regulatory agenda can be divided into a few broad categories. But over all, she views executive authority in the same broad way that Trump does. Several of her proposals are likely to end up in court — as several of his have. Here are the big areas where she has regulatory ideas. Reverse Trump administration policiesOne big chunk of her plan would reverse some Obamacare regulations established by the Trump administration. She would return funding to Planned Parenthood and other reproductive health groups that also offer abortion services, for example. She would restore funding to publicize insurance options. She would eliminate new requirements on Medicaid beneficiaries, such as work requirements and premiums. And she would change rules to restrict the sale of so-called short-term health plans, which don’t follow all the Affordable Care Act’s rules. She would restore an Obama-administration policy that provided civil rights protections to transgender patients and women with a history of abortions, among other groups. Expand benefits in existing insurance programsShe would seek to offer subsidies to new groups of people to help them buy health insurance under Obamacare, including legal noncitizen immigrants and the families of people who can obtain coverage for only themselves through work. She would also seek to add a dental benefit to the Medicare program, by reinterpreting language in the statute that says dental care can be covered only if it is “medically necessary.” And she would change aspects of the Medicaid program, making it easier for states to offer coverage to more people, even if it will cost the government more. She would write new rules for a 2008 law that requires insurers to cover mental health care in the same way they cover care for physical ailments. The goal is to expand coverage for mental illness and substance abuse across different types of insurance. Lower drug pricesMs. Warren’s regulatory agenda is perhaps most aggressive in its efforts to limit drug prices. She proposes that the federal government employ never-before-used authority to rescind existing patents on medications that were developed with the help of government funding. She would also expand an infrequently used authority so that the government itself could manufacture certain drugs in public health emergencies. Among the drugs and devices she would target are insulin, EpiPens, antibiotics and medications for hepatitis C, H.I.V. and opioid overdoses. The list of policies above does not include everything that Ms. Warren has proposed. She’d also like to beef up antitrust enforcement in health care, for example. But it gives a sense of the breadth of things she would try to do in health care, even without Congress’s help. President Trump is far from alone in failing to enact his preferred health policies through legislation. Several presidents before him have struggled to pass major health overhauls. As Democrats head into another debate next week, the moderators may want to consider asking candidates what’s on their health care regulatory wish lists. The answer may be far more useful in predicting the shape of their policy agenda than the details of their legislative dreams. Step therapy, also known as “fail first,” is a process used by health insurers to control costs. It requires patients to try one or more medications specified by the insurance company, typically a generic or lower cost medicine, to treat a health condition. The health care landscape is rapidly changing as employers, patients and health care providers look for ways to contain rising costs. But you don’t have to understand every part of this complex industry to bring about change.
Offering a health plan for your employees is a vote of confidence in that plan’s network, coverage and overall ability to improve your workforce’s access to affordable health care. Small business owners can further health care innovation by carefully assessing which plans will bring the most benefit — and the most value — to their employees. What Is Value-Based Care? For decades, the health care industry operated on a fee-for-service payment structure. If you received a service, your doctor or hospital was paid for that service, even if it wasn’t clinically necessary or didn’t end up improving your health. The value-based care model, on the other hand, aims to tie how patients pay for care to how effective that care is — in other words, how much value it brings. Value-based care has already been shown to reduce emergency department visits and inpatient hospitalizations, and it has led to improved preventive care and chronic disease management. What Role Do Employers Play? Nearly 50 percent of insured Americans get their insurance through their employers. The success of your business relies on your ability to attract and retain the best talent, which often means providing an appealing benefits package. But offering competitive benefits without straining your budget isn’t always easy. In order to properly assess health care costs, employers should understand what tools are available to control them. When choosing a health plan, look for one that includes the three pillars of value:
How Can Employers Find the Best Health Plan Solution? Many health plans tackle at least one of the pillars, but bringing them all together will give your business the best chance of delivering value in your employees’ health care. Anthem’s Cooperative Care pilot program, for example, helps employers in certain states control health care costs by rolling all three pillars into one plan. With the program, employees choose a primary care provider to act as their hub for medical services and use an ACO within a high-performance network. Specialists and other providers within the network are held accountable for the overall service they provide, with value-based payment models that reward providers for high-value/low-cost services and improved outcomes. Employees receive a health plan designed to furnish them with coordinated care, a deeper patient-provider relationship and better health outcomes with an emphasis on overall wellness. Anthem’s Cooperative Care program offers a special focus on the patient experience, with shorter wait times, lower costs and quality doctors all leading toward the goal of better health. Employers are poised to be a major force in the value-based care transformation happening across the health care industry. In choosing a plan for your employees, you’re making a claim about what you want the next health care innovation to look like — for your workforce and for yourself. Checkout the family health insurance lancaster pa plans and find the better options for your loved ones. Cosmetic surgeries can become expensive quickly, and navigating insurance after these kinds of procedures can force patients to swim in murky waters. But with a little guidance, your employees can compare prices and find the best, most cost-effective provider.
Understanding Cosmetic Surgery Costs The cost of cosmetic, or aesthetic, surgery takes several factors into account. A deeply experienced surgeon might charge more, for example, as might one performing particularly complex procedures. Undergoing a cosmetic surgery in a large city could be cost more than having it done in the suburbs. And a hospital is generally the most expensive place to receive cosmetic procedures, but many cosmetic surgeries can take place — and cost less — at outpatient ambulatory surgical centers. Surgery that’s performed for purely aesthetic reasons generally isn’t covered by insurance. More likely to be covered are medically necessary procedures or reconstructive surgeries after trauma, for instance an accident, severe burns or cancer treatment. Insurers also routinely cover surgery meant to correct an issue present at birth. And you may find that insurance will cover part of a procedure that serves both a medical and an aesthetic purpose. For example, insurance may pick up a portion of a nose reshaping if the surgery made structural changes that improved breathing. For common procedures, you can receive an estimated price for the entire episode of care, including consultation, the actual procedure and any follow-up. The American Society of Plastic Surgeons (ASPS) provides averages for routine procedures to give you a basis for comparison. Rhinoplasty typically costs about $5,100, for example, while eyelid surgery averages around $3,000. Reconstructive surgery is more complex and may require a consultation to receive an accurate estimate. How to Control the Cost of Cosmetic Surgery First, employees should always check with their insurance to see if all or part of their procedure is covered. Get any approvals needed beforehand to help streamline the claims process. Employees can also take advantage of their health savings or flexible spending accounts to cover the costs of a surgery, as long as it’s medically necessary. They may need to obtain a letter of medical necessity to receive reimbursement or provide payment through their medical savings account, so planning ahead is key. The next step is to shop around. Encourage employees to call different doctors and ask for a cost estimate. They should get a detailed list of what is included in that cost and what additional expenses they may face, such as charges for ice packs, prescription medications or other needs. Before choosing a doctor, it’s a good idea to do some research and read online reviews. From there, employees should schedule consultation appointments with their top choices. Before getting any kind of cosmetic procedure done, they should feel confident in their doctor’s qualifications, how the surgery is done and the expected recovery time. The consultation is a chance to get any questions out of the way early on. Your employees should leave the meeting knowing the answers to the following questions, as recommended by the ASPS:
Most plastic and reconstructive surgeries are scheduled long in advance of the actual procedure, so your employees have the opportunity to take their time searching for the most competitive provider. It’s possible to have a cosmetic surgery done without draining your bank account — all it takes is a little planning. Explore private group health plan and get the best plan for business, if you want to know more details then please send your queries in the comment section. Do you ever wonder why you’ve been hearing so much about the benefits of value-based care lately?
It’s not really new; it was just a long time evolving. In the late 1990s and early 2000s, researchers started seeking reasons for the overuse of health care services — often unnecessary health care services. Their findings? Misaligned incentives discouraged coordination and collaboration and encouraged a piecemeal approach to care, reports the Center for Health Care Strategies. Various organizations, including the Brookings Institution, the Institute for Healthcare Improvement (IHI) and the Patient-Centered Primary Care Collaborative, began looking for ways to align incentives to meet the Triple Aim, first articulated by IHI: “simultaneously improving the health of the population, enhancing the experience and outcomes of the patient, and reducing per capita cost of care.” The idea caught on: Reward quality and efficiency and penalize — or at least stop incentivizing — fragmented, volume-based care. The benefits of value-based care became clear, and so began the gradual transition away from the fee-for-service (FFS) model. A Brief History of Value-Based CareTo understand the evolution of value-based care, it makes sense to start with the Centers for Medicare and Medicaid Services (CMS). CMS provides a useful chart documenting the history. Notably, the move to value-based care didn’t begin with the Affordable Care Act (ACA) in 2010. If you need a starting point, it’s probably 2008, when CMS initiated the Medicare Improvements for Patients and Providers Act, better known as MIPPA. MIPPA instituted incentives for reporting quality data and e-prescribing. It set the stage for an array of other programs, all of which apply to physicians who accept Medicare, and the payments applied only to Medicare payments. In 2012:
In 2014:
And in 2015:
The ACA and ACOs The ACA accelerated value-based models; among its multitude of provisions was the Medicare Shared Savings Program, which created Accountable Care Organizations (ACOs). ACOs make participants — typically, clinicians, practices and hospitals — accountable for the health of their patients. Providers in ACOs receive financial incentives to coordinate care, reduce errors and avoid unnecessary tests and procedures. They also benefit from economies of scale. A successful ACO meets quality standards and yields savings, which are shared among payers and providers. In many models, an ACO shares risk, too: If it spends more than the targeted amount, it must repay some of the difference. Private insurers shortly followed suit, recognizing the benefits of value-based care in general and ACOs in particular. A Work in ProgressDespite all the progress with value-based care, FFS remains the dominant reimbursement model. It will likely remain so for several years, but value-based models continue to prove their value. FFS focuses on sick care — caring for patients after they become ill. The value-based care model focuses on health care and pays providers for the value of the care they provide, not the volume. And that’s the key point when considering value-based care vs. fee-for-service. Here are the main distinctions between the two models. 1. Volume vs. Value, Quantity vs. Quality Under FFS, clinicians, hospitals and medical practices are reimbursed based on the quantity of services delivered. More visits, tests and procedures mean more money. Spending more time with a patient or providing patient education hurts their income. Likewise, they aren’t paid to work with other providers to coordinate patient care. As a result, one provider doesn’t know what the other is doing, resulting in inefficient delivery and wasteful service duplication. With value-based care, payment is determined by the quality, not quantity, of services. Appropriateness of care, efficient use of resources and clinical outcomes dictate reimbursement, not how many patients can be seen in an eight-hour day. Practices focus more on advancing the Triple Aim — better care for individuals, improving population health management strategies and controlling health care costs. 2. Proactive vs. Reactive Value-based care supports proactive management of health: preventing illnesses and injuries or catching them at an earlier stage when they’re less expensive to treat. The point is to avert the use of services when possible. Providers are paid to keep patients out of the hospital and to ensure that each test is necessary. By contrast, FFS is reactive. Clinicians, practices and hospitals get paid more when patients use more services. The focus is on treating the sickness rather than keeping the person healthy. 3. Inside vs. Outside the Clinic Walls FFS focuses on what happens during the office visit or at the lab; it’s about the specific treatment or procedure. Value-based care takes a more holistic approach, looking at the patient and the patient population beyond the clinic walls. It’s proactive, focusing on prevention and even “nonvisit” care, such as providing health coaches. For diabetes, the patient might be connected with a nutritionist or set up with remote glucose monitoring. But, as the National Institute of Diabetes and Digestive and Kidney Diseases puts it rather bluntly, “Providing that care requires that a practice knows exactly who is receiving diabetes care.” That’s where data comes in. 4. Data-Driven Coordination vs. Working in the Dark In value-based care models, physicians have access not only to their own data, but also to patient data across the continuum of care (from labs to specialists, and so on). This gives them a better view of each patient and the patient population. With this data, they can identify all the patients who have a particular condition and those at risk for it. For example, that information can be used to determine which patients are at risk for diabetes. It can also be used to develop population-based interventions for every patient with diabetes. In contrast, FFS providers often lack the technology and the incentives to coordinate patient care across the continuum. Physicians are siloed, often lacking robust data on their own patient populations. And because they can’t see the tests run by other providers, they often duplicate procedures, like having a patient take a blood test for a second or third time. This coordinated vs. fragmented distinction may be the essence of value-based care vs. fee-for-service. It’s the efficient, data-supported, coordinated approach to care that delivers value by avoiding redundancy, leveraging economies of scale and working across the care continuum to keep your employees healthy. It’s health, not bean counting, that drives the savings. Visit with an online doctor from the comfort of your home and get expert advice, a treatment plan and a prescription if needed. If you have kids, you probably know that child care tends to fall through at the most inconvenient moments.
This creates a stressful problem, and a costly one, too. According to the 2017 Child Care Aware of America Report, nearly half of working parents miss on average more than eight days of work a year because of breakdowns in child care. And for employers, that absenteeism gets expensive, to the tune of about $4.4 billion a year. Subsidizing Care: A Win-Win Investment That’s why supporting working parents isn’t just a generous thing to do for employee peace of mind — it’s a good investment in your workforce as a whole. And some businesses have caught on, offering employer-paid child care benefits that tackle four main areas: affordability, access, tax savings and workday flexibility. Starbucks is one company leading the charge. In October 2018, the company announced that it would subsidize 10 days of backup child care each year for all employees. The subsidy makes backup care much more affordable for in-home and in-center services at $1 and $5 per hour, respectively. Should you join them? The benefits of time and opportunity costs saved from missed work days make a compelling business case to do so, but according to a 2016 survey from the Society for Human Resource Management (SHRM), subsidized child care is still an underdog in the world of benefits. All told, just 2 percent of employers (big and small) reported offering the benefit, dwarfed even by the number of companies that offered day care at or near the work site (7 percent). Why the lack of participation? It’s simple: Many businesses, especially small ones, just can’t afford it — even though they’d like to, and even though they realize the impact those investments could have on their bottom line. If that sounds like you, don’t despair. The SHRM survey showed that there are other ways to go about supporting working parents. Other Solutions: Tax Savings and Care Finder Services Dependent Care Assistance Plans (DCAP), which allow employees to contribute pretax dollars for dependent care — much like health savings accounts do for health expenses — topped the list. About 56 percent of all employers in the SHRM survey reported that they offered DCAPs to employees, and 49 percent of small employers (50 to 99 employees) did so. Like health savings accounts, DCAPs offer a flexible option for employers. You can help contribute as much or as little as you want to employees’ accounts, and your workers reap the benefits in tax savings. With a 41 percent participation rate, child care location services (such as offering referral resources) were also popular, according to the SHRM survey. Other options trailing behind in the minority included summer child care, sick care and backup care. And Finally: Good Old-Fashioned Flexibility If none of these solutions piques your interest or meets your budget, simply building more flexibility into the workday can do a lot to help accommodate working parents. Consider flexible schedules that work around school pickup and drop-off times or work-from-home options for when child care falls through. Because inevitably, it will — and when it does, it’s best to have solutions in place for your employees that save their sanity and your bottom line. Explore small business health insurance plans and get the best plans for your business, if you want to know more details then please send your queries in the comment section. Workplace wellness programs are a popular benefit, and for good reason — they’re an effective, engaging way to teach employees how to live healthier lives. But teaching employees how to improve their finances can be just as beneficial for their health, not to mention their pocketbooks. Here’s what your company has to gain from adding a financial education program to its offerings.
Financial Literacy and Health Financial literacy entails having the knowledge and confidence to handle money issues like managing debt, saving for retirement and setting a budget — things people need to deal with every day. Despite how important these topics are, according to Fortune, nearly two-thirds of Americans could not pass a quiz covering basic financial literacy concepts. Almost no one can say they’ve never worried about the bills, but serious financial stress can lead to health problems including depression, anxiety, trouble sleeping, high blood pressure and diabetes. Even worse, a low bank account balance might convince a sick employee that seeing their doctor or getting other important medical care isn’t worth the expense, even if they really need it. Financial stress also follows employees into work. When your employees are having trouble making ends meet, it’s nearly impossible for them to fully concentrate at work. The Society for Human Resource Management found that an employee’s personal financial issues can lead to an inability to focus at work and higher absenteeism. 4 Ways to Improve Employee Financial Knowledge If you’re interested in improving your employees’ financial skills, here are a few tried-and-true strategies to have in your back pocket.
Maximizing Health Insurance Benefits Covering your health insurance plan as part of your financial literacy training will help employees get the most out of one of the key benefits included in their package. At a minimum, you should remind everyone about how they can reduce their health care costs by looking for in-network providers, following up with preventive treatment and using generic prescriptions when possible. As you discuss budgeting, show examples of how much different trips to the doctor or hospital could cost employees under your plan’s current structure for deductibles and copays. Then, discuss strategies for how employees can save part of their income to prepare for these costs. If your health offerings include extra features like a flexible spending account (FSA) or health savings account (HSA), your financial literacy program might benefit from a workshop or seminar explaining how these more complicated programs work. For example, make sure employees know that the money in an FSA follows a “use it or lose it” policy and might be lost at the end of the year. Promoting financial wellness is a small investment on your end, but it can greatly improve the finances, health and productivity of your employees, so don’t overlook this workplace benefit in your office. When your employees are financially well, they’ll pour less of their energy into stressing over bills and more of it into making your business successful. Explore health insurance plans harrisburg and get the best plans for your family, if you want to know more details then please send your queries in the comment section. When one of your employees gets a new diagnosis, especially an unexpected one, their worrying doesn’t stop as they leave the hospital. They’ll carry that stress with them at home, as they run errands and, of course, at work.
As an employer, it can be tough to know how to help someone coping with a diagnosis — whether it’s their own or a family member’s — but as difficult as it may be, letting your workforce know you’re there to be a supportive presence could have a big impact on their mental state and their productivity and they navigate treatment and recovery. Try out the following seven tips to ensure you’re prepared to begin supporting employees through a tough time, whatever their situation is. 1. Respect Their Privacy Legally, an employee doesn’t have to tell you that they or a family member received a new diagnosis. Let them come to you in their own time to share the details, and ask how or if they want the news to be shared with colleagues. Once they’ve answered, respect their decision. 2. Direct Them to the Right Benefits Make sure the employee has someone to talk to who can thoroughly explain all of the benefits available to them, including health insurance, short-term disability, the Family and Medical Leave Act, counseling services, an employee assistance program and any other benefits you may have in place. 3. Be Flexible With Scheduling Some diagnoses might not change an employee’s schedule much, but others can require time-consuming treatments and appointments. As much as possible, discuss ways you can adjust their schedule to accommodate treatment and recovery. Can some client meetings be conducted through a video conference rather than in person? Can the employee work from home during specific treatments or during their overall recovery period? Can their core hours be shifted to accommodate appointments? 4. Create a Plan for Work A newly diagnosed employee might worry about not getting all their work done, but that kind of added stress will only slow down their recovery. Take the lead in developing a schedule to determine what tasks need prioritizing, what can be delayed and what should be delegated to someone else. 5. Give Them Space Answering calls from a doctor about test results or other confidential medical information can be awkward in an open office environment, especially if an employee is keeping their condition private. Offer up your office or another quiet, separate area as a space to take phone calls. Small gestures like this can do a lot to maintain morale and make your entire staff feel supported. 6. Guide Co-Workers in How to Help If the employee chooses to share their diagnosis with others, they may find themselves overwhelmed as everyone jumps in to help. While your employees’ thoughtfulness is obviously a positive thing, try to direct their energy in a more useful way. Ask what would be most beneficial to the employee with the health concern, and tell your staff how and when they can assist. For instance, you might send around a sign-up sheet with different opportunities to help, such as bringing in a meal, doing chores, donating vacation hours or raising money to cover medical costs. That way, their efforts will all go toward the right things. 7. Check In With Encouragement Calls, texts or cards just checking in and hoping for a quick recovery let the employee know you care. Just make sure not to mention work — there’s a better time and place for those conversations (namely, at work). Work is a source of stress for many Americans — but when an employee is facing a new diagnosis, you can flip the script and turn the workplace into somewhere they feel supported. This can improve morale, giving the struggling employee an emotional boost that can aid their recovery. As an employer, you have an opportunity every day to decide what kind of business you want to run and how it treats the people who work to keep the company successful. It just makes sense to make coping with a diagnosis as easy for them as possible. Explore business health insurance plans and get the best plans for your company, if you want to know more details then please send your queries in the comment section. As an employer, your health care costs are likely to rise in 2017, according to the National Business on Group Health Plan. But, by how much? In some ways, it’s up to you. The health insurance marketplace will evolve and change, but it’s unlikely that the direct costs or insurance premiums are going to decrease. The year-over-year increase that you pay, as the sponsor of a health care plan, comes down to regular analysis and review of plan selection and use.
Your company’s health care costs are primarily defined by the plans you offer to employees. And for employers that insured employees for decades, the idea of eliminating the most expensive plan option may feel heartless. Some of your employees have grown to depend on the doctors they see who accept that one plan. But those doctors likely accept other plans. And as long as you offer other, more affordable plans, you could consider paying a smaller percentage of that high-end plan, especially if times are tight. Review Your Current Enrollees Review your participant list and ensure everyone still qualifies for your health benefit. If you have a few employees who have gone through a divorce, you could still be paying for the ex-spouse’s insurance. Respectfully ask they exit the plan. While employees really value dependent coverage, keep in mind that you’re not required to offer or pay health insurance costs for any partners, spouses or dependents. And with other insurance potentially available for those family members, consider reducing how much of those costs you’re willing to cover. Consider Offering a High-Deductible Plan Consider offering plans that have high deductibles and high out-of-pocket limits. These are great options for a young, healthy workforce unlikely to visit the doctor much throughout the year. Health insurance plans usually include a free annual physical, so encouraging your healthy staff members to consider these kinds of minimal coverage plans won’t discourage them from critical, preventive care. In addition, you can encourage your employees to buy supplemental plans that will help them cover out-of-pocket costs and living expenses in the case of a serious accident or illness. The high-deductible health insurance plan covers the majority of the health care costs, and the supplement insurance can cover many out-of-pocket bills. Create a Wellness Program Jump on the preventive care bandwagon. By encouraging preventive care like flu shots, annual physicals and cancer screenings, you’ll create a culture in your workplace that values healthy living. Will a healthier workforce really translate to lower insurance premiums? In short, yes. If you have a workforce that’s routinely sick, your health insurance contract prices will rise faster every year. But more importantly, by encouraging healthy living and preventive care, you’ll have a more productive workplace. Employers with healthy employees have higher productivity, fewer sick days and lower turnover. The real savings could come in the form of offsetting other costs. Don’t ignore your health insurance costs. You need to invest your time in revising your company’s health plan options, reviewing plan use by employees and encouraging preventive care. You aren’t at the mercy of rising health care costs. You’re a driver of those costs, and you can steer your company in a better, leaner direction. Currently, 23 states and the District of Columbia have legalized medical marijuana. Despite the fact that medical marijuana laws vary from state to state and clash with federal law, most state prescriptive marijuana laws protect both eligible patients and their primary caregivers. According to an article by the National Council of State Legislatures, patients who have their physicians’ permission to use marijuana to treat a chronic illness or relieve symptoms may be protected from arrest in some states.
In light of the above, employers may be contemplating whether they should accommodate employees who have been certified to use marijuana medicinally. An article on the Blog for Business Law noted that the Americans with Disabilities Act (ADA) calls for employers to provide reasonable accommodation for certified employees with a disability. These include prescribed marijuana users who are authorized as disabled under state law. Prior to making reasonable accommodation for a registered medical marijuana employee, you may want to reflect on the following strategies: Clear Written Policy It’s vital you first closely follow the legal requirements of the state and relevant federal regulations when writing your company’s policy on prescriptive marijuana accommodation. Involve your human resource personnel and acquire legal advice from an expert on the specific state laws to draw up a clear and comprehensive policy. Reflect on Risk Threshold You may want to include in writing prohibiting marijuana use or possession at work and circumstances resulting in employee termination, such as failure to fulfill job responsibilities or posing safety issues towards others. Since termination should be regarded as a last resort, the following actions may be taken if marijuana use results in impairment:
The employee concerned can be subjected to consistent monitoring to safeguard workplace standards and safety. Effective, Ongoing Communication A company that communicates transparently and collaboratively with its staff on an ongoing basis shows its interest in achieving shared goals. This also prevents unnecessary disputes in the long run. Include one-on-one, informal communication with the employee to clarify any area in the policy that he or she lacks understanding of, communicate expectations and prohibitions on marijuana use, gather feedback on how the employee is coping with work responsibilities and recommend any alternative job areas. Undeniably, all information will have to be kept confidential. Publishing your policy on the company’s intranet is also a way to encourage open communication so concerned employees are clearly informed of the processes and requirements they need to observe as well as expectations they have to meet. Laws surrounding medical marijuana may change from time to time. It’s important to keep abreast of legal developments in your state and align your company’s policy with current state laws. According to an article in the Minneapolis Star Tribune, by constantly reviewing your company’s guidelines and regularly educating your employees, you’ll be confident that medical marijuana use is handled in a relevant, consistent and transparent manner throughout the organization. There are various health insurance companies in pa, which provides best health insurance for small business owners and if you want to know more then please drop your comments. Don't let the end of your marriage derail your savings or reduce your Social Security benefits.
When it comes to retirement, divorce can be disruptive at best and devastating at worst. This is especially true of divorce after age 50. Spouses are at risk of losing a significant amount of their retirement savings and may have relatively few years left to replenish their accounts. "Both spouses have to adjust, but the spouse with the lower income has to adjust more," says Nicholas Yrizarry, president and CEO of investment firm Align Wealth Advisors in Laguna Hills, California. He recommends divorcees move forward by stepping back, regrouping, restrategizing and re-implementing their retirement plans. Take the following steps to retool your retirement plan after getting a divorce:
Ensure You Have a Proper Qualified Domestic Relations Order If your spouse has an employer-sponsored retirement plan, nothing may be quite as important as obtaining a Qualified Domestic Relations Order, otherwise known as a QDRO. "QDROs are orders that qualified plans require in order to pay out nonparticipants," explains Dana M. Stutman, a founding partner of the matrimonial law firm Stutman Stutman & Lichtenstein, LLP in New York City. In short, the only way to get a payout from a 401(k), pension or similar plan if you're not the worker is if you have a QDRO. However, QDROs need to be written in a certain way to be accepted. "The (retirement) plan administrator may have very specific rules," Stutman says. Because of the complexities of these orders, they can be time-consuming and expensive for an attorney to draft. A more cost-effective option may be to employ an actuary who specializes in writing QDROs, Stutman suggests. The nonparticipating spouse can take money received from a QDRO and roll it into his or her own IRA or other retirement fund. Before taking that step, consider whether you will need any of the money for another purpose. In most cases, people are assessed a 10% penalty if they withdraw money from a tax-favored retirement plan prior to age 59 ½. However, you can take proceeds from a QDRO without a penalty, says Shelby J. Smith-Beckert, senior financial consultant with Orlando-based International Assets Advisory. You'll need to make the withdrawal prior to rolling the money into another retirement account though. Understand Your Spousal Benefits for Social Security A divorce doesn't necessarily mean you lose out on Social Security spousal benefits. So long as you were married for 10 years and have not gotten remarried, you are entitled to receive retirement benefits from your ex-spouse's Social Security record. If you start receiving benefits at your full retirement age, you'll receive an amount equal to one half your ex-spouse's full retirement benefits. If you claim benefits early at age 62, you'll get a reduced amount. However, your ex-spouse will need to be at least 62 as well for you to begin claiming benefits, and unless he or she is already receiving Social Security benefits, you'll need to wait two years after your divorce to begin payments. Claiming these benefits in no way affects your ex-spouse's retirement benefits or that of anyone he or she marries after you. Create an Inventory of Investments and Assets Now that you understand what, if any, retirement funds you'll receive from your ex-spouse, it's time to take a complete inventory of your assets. While an inventory may be provided at the end of the divorce, it's important to review and verify this information, says Bryan Bibbo, an accredited investment fiduciary with advisory firm The JL Smith Group in Avon, Ohio. "Maybe your ex-spouse was the one handling the finances," Bibbo says. Take this time to familiarize yourself with your accounts and their tax implications. If you're confused, seek a financial professional for guidance. "Usually, when I'm dealing with divorced individuals, I'm doing a lot of education," Bibbo says. For instance, people may not understand how 401(k) payouts are taxed and whether it makes sense to request a lump sum or periodic payments from a retirement plan. Update Your Retirement Plan A retirement plan for a married couple should take into account the ages, goals and incomes of two people. When you become single, you need to consider whether the plan meets your needs. You may have to adjust your portfolio to better reflect your expected retirement date and personal risk tolerance. At the same time, update the beneficiaries on all your financial accounts. "The beneficiary designation takes precedence over your will," Smith-Beckert says. Unless you want your ex-spouse to receive your money, make sure his or her name is removed from all retirement funds, life insurance policies and other accounts. Start Contributing to Your Own Savings If you aren't already, now is the time to budget money for your future. That means creating an emergency fund that can cover three to six months of expenses, plus setting aside an adequate amount for retirement. "You want to have a written plan with your goals," Bibbo says. Every situation is unique; he recommends working with a financial planner to choose the right mix of retirement accounts and other savings vehicles to meet those goals. Adjust Your Lifestyle as Needed Perhaps the most difficult aspect of divorce is that it often requires people to make significant life changes going forward. "They don't realize how much divorce should impact their lifestyle," Yrizarry says. That may mean downsizing a house, forgoing vacations or changing jobs to pay bills and save enough for retirement. These changes can feel disheartening and overwhelming, but Yrizarry says surrounding yourself with positive people can help. Seeing changes as opportunities for improvements rather than setbacks can also make these adjustments more manageable. With the right attitude, Yrizarry says people can go through a divorce and come out of it stronger in the end. It is important to have health insurance for any individual and you can check your eligibility for group health insurance and explore best plans for you. Avoid high medical costs by using Medigap insurance to cover what Medicare doesn't. Medigap policies are extra insurance you can buy if you have Medicare. These plans are designed to help pay for some of the costs that are not covered by Medicare Part A and Medicare Part B. “Original Medicare leaves deductibles, copays and coinsurance behind for the beneficiary to pay for approved medical care and services,” says Danielle K. Roberts, co-founder of the insurance agency Boomer Benefits in Fort Worth, Texas. With a Medigap policy, you could potentially save thousands of dollars in medical bills. Here’s a look at how Medigap insurance works, what to consider when choosing a policy and the best time to enroll. What Is Medigap? A Medigap plan is a private insurance policy that can help you pay for some of the out-of-pocket costs associated with traditional Medicare and sometimes additional services. You must pay a premium for Medigap insurance in addition to your Medicare Part B premium and Medicare Part D prescription drug premium. Who Is Eligible for a Medigap Policy? To qualify for Medigap, you’ll need to have Medicare Part A and Medicare Part B. In general, individuals who are 65 and older are eligible for Medicare. If you have a Medicare Advantage plan, which is sometimes referred to as Medicare Part C, Medigap coverage is not available. What Medigap Covers Medigap plans are designed to supplement Medicare coverage. There are a variety of different Medigap plans, and each one is identified by a letter. You’ll find Medigap plans including A, B, D, G, K, L, M and N. Each plan is set up to provide a different level of supplemental coverage to Medicare. “Different plans cover different things,” says Lev Barinskiy, an insurance comparison website. To see the exact benefits for each plan, it can be helpful to look at a plan comparison website, such as the one provided at Medicare.gov. A key advantage of Medigap policies lies in the network of health providers you’ll be able to visit. “A Medigap policyholder can see any doctor who accepts Medicare,” says Shaun Greene, head of business operations at Health Pocket. Medigap plans only cover one person, so if you’re married, you and your spouse will need to purchase separate policies. The plans do not cover prescription drugs, hearing aids, vision services, dental care or long-term care. How to Select a Medigap Plan Medigap policies are standardized, and each insurance company must offer established benefits for each plan. This means a Medigap plan with a given letter will be the same anywhere you buy it. “The only difference is the price,” says John Hill, president of Gateway Retirement in Rock Hill, South Carolina. "In every state, there are many companies offering the same coverage at a different price." When choosing a plan, you’ll want to think about your budget and health factors. “If you are pretty healthy and don't go to the doctor often, Plan N may be a more cost-effective option than Plan G," Roberts says. "If you go to the doctor once a month, Plan G would likely be more cost-effective than Plan N." If you travel abroad frequently, you might opt for a plan that covers emergency services in other countries. Once you know which plan will be best for your needs, you can compare prices among insurance companies and also read company reviews. “Compare premiums, average rate increases and financial ratings of the carriers,” Roberts says. When to Enroll in Medigap You can sign up for a Medigap plan during the six months after you enroll in Medicare Part B. During that time, you can purchase any Medigap policy that is sold in your state. Even if you have health problems, it's guaranteed that you'll be accepted, and insurers won't charge you more based on your medical conditions during this initial enrollment period. After six months have passed, you will no longer have the guarantee that your application will be accepted. Insurance companies might not grant you a Medigap policy and group health insurance plans if you have certain health conditions. Even if you are able to buy a Medigap plan, it may cost more. While health care costs take many different shapes, your employees probably associate them most closely with the premiums they pay for their insurance. That said, they may not know everything they should about this piece of the puzzle.
Who sets the price? Where does the money go? Are health insurance premiums tax deductible? Here’s a look at some common questions your employees — and you — might have about your premiums. What Are Insurance Premiums? A premium is what you pay to keep an insurance policy active. In exchange for this fee, the insurance company agrees to cover some or all of your medical bills. Monthly premiums are the most common type, but you can also make larger payments less frequently, for instance once a quarter or once a year. The insurance company collects premiums from its customers to cover their future health care bills. Where, exactly, does the money go? The vast majority — roughly 82 cents of each dollar — goes toward medical expenses like prescription drugs, doctors’ services and hospital visits. The rest of the premium is split between taxes, operating expenses, claims administration, providing technology and the insurer’s profit. How Do Insurers Set Premiums? Insurance companies can’t just set any price they think consumers will pay; the government regulates what they charge. Under the Affordable Care Act (ACA), insurers can only base their premiums on the following five factors.
If an insurance company wants to increase premiums for the next year, they need to apply for approval from the insurance commissioner’s office and prove that either medical costs have gone up or their losses were higher than expected. Are Health Insurance Premiums Tax Deductible for Employers? Whatever you pay for employees’ health insurance should be tax deductible for your business. This applies whether you pay the entire premium or split the costs with employees. The share your business pays counts as a tax deduction. You can also deduct any contributions to employee accounts to help them cover medical expenses, like a health savings account or a health reimbursement account. If your organization uses any of these accounts, giving extra money to employees will earn you a tax break. For the time being, there is no limit on the employer tax deduction for insurance premiums. While the ACA originally set a penalty for employers paying for plans that were overly expensive known as the Cadillac tax, the government delayed this tax until at least 2022, according to Forbes. For now, whatever you pay for employee premiums is fully tax deductible. Are Health Insurance Premiums Tax Deductible for Employees? Whether premiums are tax deductible for your employees is a little less certain; it depends on how they get their coverage. If you provide a group plan at work and they use that, then their premium payments may be deductible. Intuit notes that payroll typically takes premiums out of employees’ pretax income, meaning the tax break already applies — your employees have less taxable income, which has the exact same effect as claiming a tax deduction when they file their return. It’s only if your payroll lists the staff’s premium payments as wages that employees should claim a tax deduction for their premiums later. That said, this setup is rare. Chances are, your payroll has taken care of the tax break for employees by taking premiums out of their pretax income. What About Employee Coverage Outside of Work? On the other hand, if your employees get their health insurance outside of work, it’s more difficult to qualify for a tax deduction. First, they need to itemize their deductions rather than claiming the standard deduction. Second, starting in 2019 they will only receive a tax deduction if all of their medical expenses, including premiums, exceed 10 percent of their adjusted gross income (AGI), according to Intuit. For example, if an employee has an AGI of $50,000, their medical costs must be more than $5,000 for anything to be deductible. The first $5,000 of costs will not be deductible — only expenses added on beyond that amount. If their total medical expenses including premiums are $5,500, they will only have a $500 deduction. Since employees might have trouble deducting premiums outside of work, this is one more reason setting up your own group plan can be beneficial. Even if you don’t cover the premiums yourself, your employees would benefit from the tax break. The government created a sizable tax deduction for Group health insurance premiums, especially for workplace plans. By taking advantage of all these benefits, you can make coverage a little more affordable for yourself and employees. When it comes to knowing what “runs in the family,” your employees probably have a scattered recollection — like remembering that Aunt Irene had some type of heart issue or that Grandpa Joe had lung cancer.
Beyond that, memories tend to get a little fuzzy. Aunt Irene’s heart issue might have been the result of a congenital defect she had since birth, for example, while Grandpa Joe may have been a lifelong smoker. Here’s why it’s important to get the details right. The Value of a Family Health History Without a written family health history that tracks these kinds of details, your employees might not have the information they need to make decisions about early screenings, genetic testing or lifestyle changes, according to the Mayo Clinic. That increases the chances that an employee will develop an unchecked chronic condition like cancer, heart disease or diabetes, something that will both change that worker’s entire life and impact your bottom line. According to the Centers for Disease Control and Prevention, each employee with a chronic condition costs employers about $1,685 annually in missed work. While simply keeping a detailed family health history won’t necessarily prevent chronic issues (or absenteeism), it can help employees take precautions to stay healthy, as well as serve as a great tool to bring to checkups and discuss with their doctor. But where do they begin — and how can you help? Start by pointing them to the U.S. Surgeon General’s My Family Health Portrait. The comprehensive form has a space to fill out medical issues for each member in the bloodline, which will give employees a composite view of their family history. Who — and What — Should Be Included? The more relatives included in a family history the better. The U.S. Surgeon General recommends starting with immediate family members: parents, siblings and children. Then move to grandparents, aunts, uncles, nephews, nieces and half-siblings. Less crucial are cousins, great uncles and great aunts — but if there’s a way to get their information, it can only help. Once equipped with the U.S. Surgeon General’s form and a list of relatives, your employees are ready to get started. Encourage them to think through medical history questions in advance to reveal potential problems that might be hereditary, such as:
Remind employees not to overlook issues relating to mental health or substance abuse. While they can be touchy topics, conditions like depression and alcoholism can increase the risk of other issues. Spotting Red Flags As employees dig into their family histories, they might notice patterns emerging, such as relatives who died at early ages or diseases that seem to run in the family. Some patterns may be simple coincidence, but others could pose a red flag worth mentioning to their doctor.
If you launch a family health history initiative, you’re bound to be asked, “Will this impact my premiums?” To ease concerns, reassure employees that this information is theirs and theirs alone, and that it won’t negatively impact their cost of care. Instead, convey that it’s a tool for them to manage their health in a more informed way. And that’s a whole lot better than an uncertain recollection of Grandpa Joe’s health. Get the all information about small business group health insurance by sending your questions in the comment section. When deciding what types of health plans to offer your employees, you have a lot of choices. Employees may already be familiar with traditional
Health Maintenance Organization (HMO) and Preferred Provider Organization (PPO) plans, but what about Exclusive Provider Organization (EPO) plans? Here’s what makes EPO insurance plans unique — and how to determine whether or not your employees could benefit from having them as an option. What Are EPO Insurance Plans? With an EPO plan, the insurer negotiates payment rates with a targeted network of physicians, usually in the local area. This may mean that they develop a network of physicians within a certain regional health system, for example. As the name implies, those who choose an EPO group health insurance plan must stay exclusively within their network for physicians, hospitals and specialists to have their care covered. How Do EPO Plans Compare to Other Plans? Two of the more common plans, HMOs and PPOs, have their own restrictions concerning out-of-network care. Both plan types contract with a network of providers and offer lower costs to subscribers who see doctors within that network. An HMO may require that you have a primary care physician who coordinates your care — and that you get referrals from that primary care doctor before seeing specialists. The plan doesn’t cover out-of-network care (though it does make occasional exceptions for emergencies). Meanwhile, a PPO doesn’t require patients get a referral to see specialists and often covers out-of-network care, just at a higher rate than in-network care. You can think of an EPO as a sort of hybrid between these two plan types, with one major difference that sets it apart from both — the size of the network. If you have an EPO vs. HMO or PPO plan, your network of physicians will be much smaller. Just like with an HMO, you won’t receive any coverage from your insurance if you go outside the network for care other than in an emergency. While you’ll also need preapproval for hospital stays and certain services, EPOs don’t require referrals to see specialists. What Are the Advantages of an EPO? As you and your employees look at ways to limit health care costs, an EPO can be an affordable alternative to traditional plans. The biggest advantage EPO patients see is financial — EPOs typically have lower monthly premiums that other plan types. The insurer also has more leverage to negotiate lower costs by bringing subscribers to physicians and facilities in the network, which means your employees will likely pay less out of pocket. EPO patients also have the option of choosing a high-deductible plan with even lower premiums. Some employees might discover that doctors they have established relationships with are outside of their EPO network — in which case they would have to choose a different plan type, see a different doctor or pay the full cost of visits to their preferred out-of-network doctor. However, because an EPO’s network is made up of a closely organized group of physicians, many people who choose an EPO plan may find superior coordination of care as doctors make recommendations based on a deep knowledge of both their patients’ situations and their colleagues’ specialties and skills. If you offer an EPO to your employees, be sure they fully understand what the plan means. Let them know:
With a strong understanding of an EPO compared to other plan types, your employees can make an informed decision about which plan offers them the best balance of coverage and cost savings. |
Author
Archives
January 2020
|