|
Medicare’s Fall Open Enrollment is here! Officially known as the Annual Election Period (AEP) which runs from October 15 through December 7, this is main time when you can change your coverage. All changes are effective January 1 next year. If you are in a Medicare Advantage plan, you can switch plans or disenroll and return to Original Medicare. Similarly if you’re in Original Medicare and would like to join an MA plan, you can. You can also join, disenroll from or switch Medicare Part D prescription drug plans.
Each year, Medicare health plans and Part D prescription drug plans can change their premiums, deductibles, cost-sharing and some benefits, or discontinue their coverage altogether. Therefore it’s good to be aware of how your plan may change, and prepare accordingly. Some helpful preparation tips include:
To review your coverage options for 2020, you can:
2 Comments
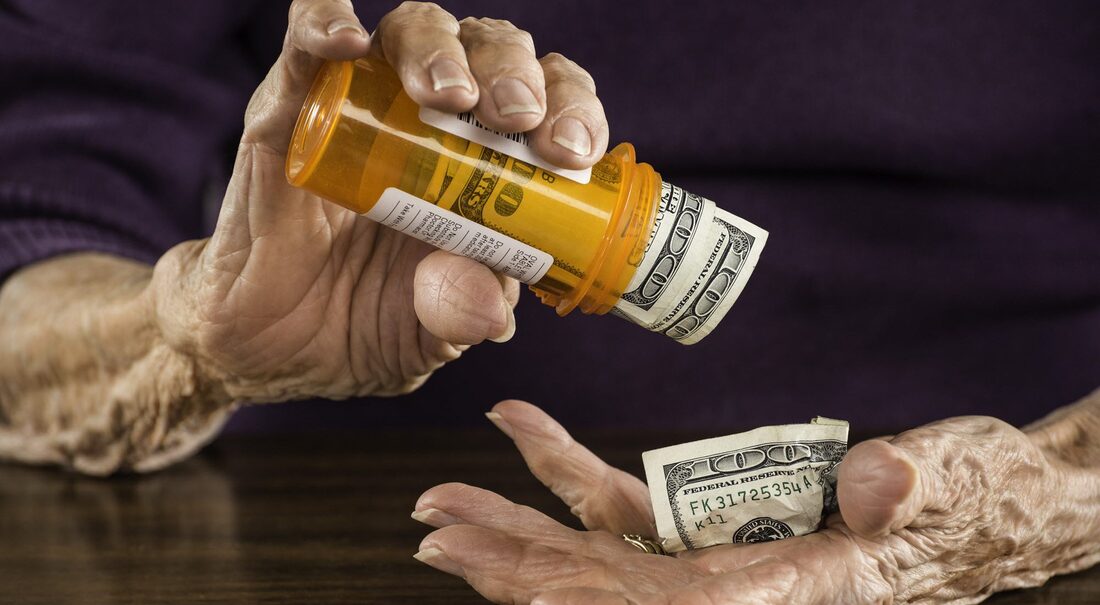
Did you or someone you work with fall into the Medicare Part D “donut hole” this year?
The donut hole, or Part D coverage gap, occurs when a person reaches a certain spending limit for their medications ($3,820 in 2018), and must pay more of the costs after crossing that threshold. Here’s how you can try to avoid the donut hole altogether and get financial assistance if you do fall into the coverage gap. The importance of shopping aroundThe Annual Enrollment Period for Medicare Advantage and Part D plans runs October 15 – December 7. During this time, people with Medicare can join, switch, or leave plans. This Part D plan checklist, developed for NCOA by the Medicare Rights Center, provides a list of questions to ask before selecting prescription drug coverage. Aside from looking at costs, you also want to make sure that you choose a plan that covers all/most of your medications and makes it convenient for you to obtain them. Using the Medicare Plan Finder, you can enter your prescription information and compare plans to determine what your costs may be in the coming year, including when/if you would expect to fall into the donut hole. Some plans may offer additional coverage during the coverage gap, like for generic drugs; however, they may charge a higher monthly premium. Working with an unbiased counselor, such as those at your State Health Insurance Assistance Program (SHIP) can help. Or use the questionnaire at NCOA’s My Medicare Matters to get recommendations about your coverage options. Isn’t the donut hole closing in 2019? You may have heard that the Affordable Care Act set in motion plans to close the Part D coverage gap by 2020, which was advanced a year in recent Medicare legislation. But “closing” does not mean that people reaching the donut hole do not pay anything for their drugs—it means that plans and pharmaceutical companies pick up more of the tab. Beginning in 2019, Medicare beneficiaries enrolled in Part D prescription drug plans reaching the donut hole will still pay 37% of the costs of their generic medications, and 25% of the brand-name medications. Getting help in the gapIf you cannot avoid the donut hole, you’ll want to explore these options to help pay for your prescriptions:
You can use NCOA’s free, comprehensive screening tool Benefits CheckUp to see if you qualify for any of these and other money-saving benefits. Avoiding the coverage gap entirely If you have limited income and resources, you may want to see if you qualify to receive Medicare’s Extra Help/Part D Low-Income Subsidy. People with Extra Help see significant savings on their drug plans and medications at the pharmacy, and do not fall into the donut hole. No matter which off exchange health insurance you choose, the prices of health insurance will always be the same. A new opportunity to switch Medicare Advantage/Part C plans is happening right now. The annual Medicare Advantage Open Enrollment Period (MA OEP) which runs from January 1 to March 31 offers anyone enrolled in a Medicare Advantage plan an opportunity to either:
Think of the Medicare Advantage Open Enrollment Period as an exchange period. Typically, when you enroll in a Part C plan during the Annual Election Period (October 15 – December 7) you have to keep the plan for the entire year until the next election period. However, with the MA OEP if you enroll in a plan that doesn’t fit your needs you can switch immediately after your new plan becomes effective on January 1. Once you select a new Part C or Original Medicare plan, your new plan becomes effective the month after your switch. You are only allowed to switch once time during the annual MA OEP. You may ask, “why go through the trouble of searching for another Medicare Advantage plan again?” and the answer varies depending on your situation. You may have enrolled in a Medicare Part C plan in October, started using it at the beginning of the year and realized that the doctor you want to see is not in-network, or your out-of-pocket costs were higher than expected. Maybe you want freedoms not offered by MA plans like visiting any Medicare-approved doctor regardless of networks. Whatever the reason, you now have an opportunity to do so without facing any penalties. If you decide to switch to Original Medicare and enroll in a Medigap plan check with your State Health Insurance Assistance Program for Medigap enrollment information. Two Opportunities The Medicare Advantage Open Enrollment Period consists of two separate periods in which you can switch plans. The previously discussed period was the annual Medicare Advantage Open Enrollment Period (MA OEP) which runs from January 1 to March 31. There’s also an individual Medicare Advantage Open Enrollment Period that varies depending on when you first enroll in Medicare. The difference between the two periods is this:
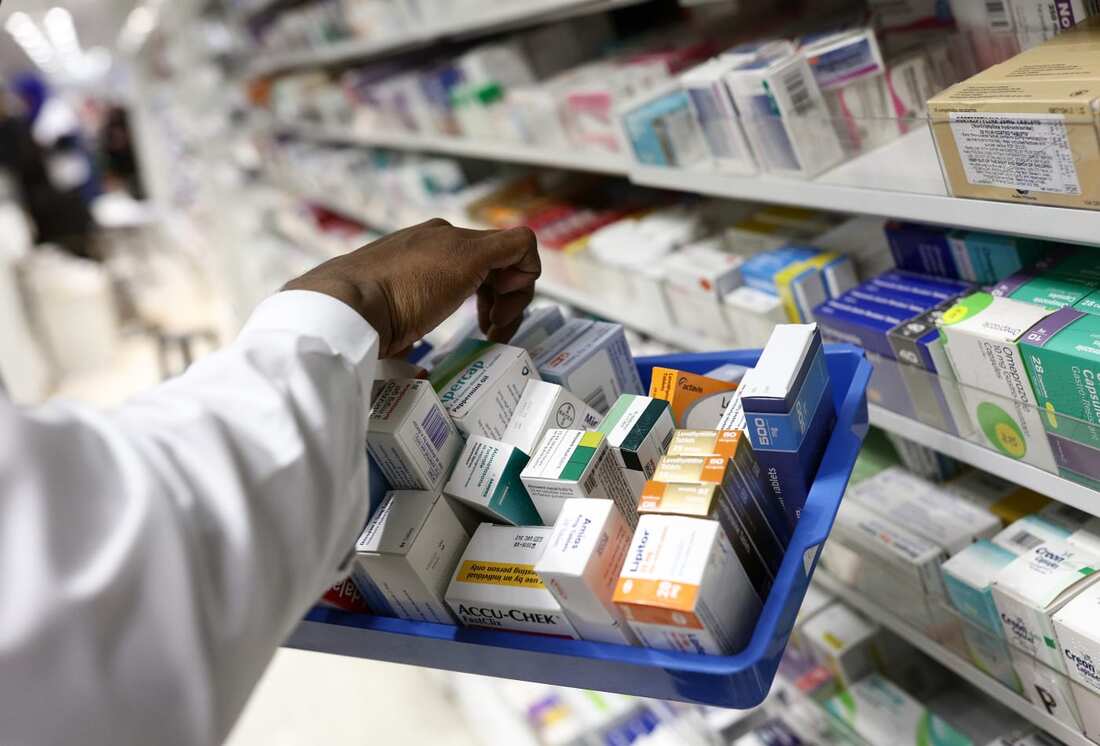
Both periods offer the same enrollment options, either switch from one Part C plan to another, or switch from a Part C plan to Original Medicare and add Part D prescription drug coverage. The only difference is when you’re allowed to do so. How to use the MA OEP Similar to other enrollment periods, to start searching for a new Medicare Advantage plan we recommend you start by taking our Medicare Questionnaire, created by the nonprofit National Council on Aging. You’ll get free Medicare advice from a licensed Medicare benefits adviser or local State Health Insurance Assistance Program (SHIP) to help you figure out your options and choose a new plan. Before you speak with a healthcare exchange pa expert figure out what questions you should ask to find the best coverage for your needs. Getting the best price: how filling a prescription is like filling your gas tank.You’re running low on gas, and there are two gas stations nearby. Do you stop at the closest one? The one with the best coffee? Or the one advertising the lowest price? If you’re like me, lowest price usually wins.
Getting a prescription filled is a lot like filling your gas tank. Did you know that prices vary from pharmacy to pharmacy for the same medicine? And, these prices can change often. Also, similar to the gas stations, the larger, well-known pharmacy chains don’t necessarily have the most competitive prices. Just like gas stations, pharmacies can set their own prices for medicines. They just have to stay within a certain range determined by the type of medicine it is and agreements they have with your particular health insurance plan. Manufacturing shortages and supply issues can also affect medicine prices – just like oil prices. The bottom line? If you’re spending a lot of money to fill regular prescriptions, it pays to find the best deal. 2 ways to shop for the best prescription cost with Medicare Unlike gas stations, pharmacies don’t post their prescription prices on brightly lit signs out front. But there are still ways to find out how much your medicine will cost before you make the trip.
5 ways to lower your medicine costsSometimes, like in the case of a medicine shortage, it’s just not possible to get a better deal. That’s when you could talk to your doctor about making a change. Here’s what you can ask your doctor about: 1. Instead of ordering enough for 90 days, can you order a 30-day supply? The price of the medicine might go down in a month or two. Then you can go back to purchasing a larger supply. However, don’t skip months or days to save money. 2. Is there a different version of the same medicine? For example, if you’re taking an extended-release version of a medicine once a day, you could try a less expensive, immediate-release version twice a day instead. The cost savings might make up for the inconvenience of taking two doses. 3. Is there a generic or preferred version of the same medicine? By law, generic versions of a medicine must use the same active ingredients and meet the same quality and safety standards as the brand name medicine. Generics are typically less expensive. 4. Is there someone who can help me look at all of my medicines? If you’re taking more than one medication regularly, consider scheduling a visit with a Medication Therapy Management (MTM) Pharmacist. These clinical pharmacists work closely with your doctor to look at your medicines, separately and together, to see how your medicines interact with each other. They can suggest less expensive versions of the medicines you’re taking and work with your doctor to see if you might be ready for a lower dosage. 5. If you have sticker shock at your pharmacy counter, let the pharmacist know that you need to get more information about the cost. Then, call your health insurance company. They’ll be able to help answer your questions and let you know if there are less-expensive options available to you. You or your pharmacist can also work with your doctor to find other off exchange health insurance options. You wake up on Jan. 1 to a new year, full of new possibilities and with it, a new amount you have to pay for your medicines before your health or drug plan helps. This is called your deductible. Your deductible resets at the beginning of each year and is the amount you’ll need to pay before your insurance kicks in.
Read on for tips about how to prepare when you are at the pharmacy counter and unexpectedly have to pay full price for your medicines. Try these tips to avoid sticker shock
Prepare now for next year’s resetThe good thing is now you know your deductible resets each year. Planning for your medicine costs to be higher at the beginning of the year can help you budget.
“Is this covered?” It’s one of the most common questions I get from members wondering about seeing a new doctor, changing medicines or trying a new treatment option. And I’m glad they call and ask me. Knowing what appointments, tests, screenings and other services your Medicare plan coverage pays for is the first step to understanding how much you’ll have to pay for your health care.
What “covered” meansIf something is “covered,” it means your Medicare plan will help you pay for it. How much the plan pays depends on the type of care you use and where you get it. To get the most cost effective health care, you’ll want all the services you use to be covered by your Medicare plan.
Checking what’s covered Keep these areas in mind when checking coverage for each plan: DoctorsMedicare plans cover specific doctors, specialists and clinics, often referred to as a network. There are ways to find quality doctors who also offer the most coverage when you see them.
Medicines Plans have a list of medicines, called a formulary, which shows what medicines they cover. The list can give you a general idea of what you may pay for your medicines.
Different medicines are covered differently. For example, generic medicines are usually less expensive than brand-name medicines. So ask how much you’ll have to pay, and make sure it fits your budget. If it’s too expensive, your doctor can help you find a different drug, or the pharmacy might have a rewards or payment program. Services From doctor visits and physical therapy sessions to blood tests, X-rays, ambulance rides and hospital stays, Medicare plans cover health care services differently.
Healthcare exchange pa plans should only be considered by people who are in good health and who do not frequently use medical services. If you want to know more details please contact us. We’re living in the digitally connected 21st century! There is more information about Medicare online than ever before. So where do you start? How do you weed through it all when you’re researching and shopping for a plan?
The Medicare Plan FinderI talk to members all the time who want to know the best online tools to search for and sign up for a Medicare plan. Right away, I tell them to check out the Medicare Plan Finder. The Medicare Plan Finder allows you to really compare your health plan options. It’s a good place to start your research. Unlike the private Medicare plan sites, Medicare.gov looks at everything across all Medicare plans. You’ll be able to see and compare how Medicare plans stack up against each other. Once you find a plan that suits your needs or at least piques your interest, use the private health plan sites to get more details. Dig deeper to check benefit levels – a benefit level is the maximum amount a health insurance company agrees to pay for a specific covered benefit. And learn more about plan offerings and any extras that may be included such as fitness benefits or discounts. Does my doctor accept my Medicare plan?If it’s important to you to keep your favorite doctors, visit Physician Compare to find your provider. And when it comes to private plans, you’ll want to see what doctors are covered by the insurance plans you’re interested in. Providers who accept Medicare may be listed as “Medicare certified” or “accepting Medicare assignment.” Be safe and secureTake the same online precautions you would when you’re shopping for anything else online. Never sign anything or give out your personal information unless you’re sure you’re on a secure web site. Doing your Medicare research has never been easier – you can learn a lot online about your Medicare options. What’s most important is that you know what you’re shopping and signing up for, and that you get the plan that best fits your wants and needs. Off exchange health insurance plans offer the same sorts of coverage that are available with ACA plans. If you want to know more details please visit us. Since I live in the Midwest, where “polar vortex” is actually a thing, I’ve always dreamed of spending the winters somewhere warm. I know a lot of Medicare members are in the same boat. Maybe you want to get away to the beach or the golf course, or just be closer to your grandkids. Wherever you want to go, it’s important to know if your health care needs are covered.
What is a Medicare Advantage travel benefit?A lot of people choose to get their Medicare benefits through a Medicare Advantage plan. One of the benefits of this kind of plan is that you can save money on health care costs if you see doctors, clinics and hospitals that have agreed to provide plan members with health care services (called a network). If you’re spending part of the year away from home, here are a few things to keep in mind:
With a travel benefit, you’ll pay almost the same for care out-of-state as you would close to home. The benefits and costs are different for every plan, so you’ll need to do your homework to figure out what’s best for you. How does a travel benefit work? Some travel benefits, such as those for international travel, are based on where you’re going. Others cover you for a certain time period — say December through April at your home-away-from-home. So a benefit like this might get you the same services for roughly the same out-of-pocket costs you’d pay at home. It’s pretty common for your health plan to require that you be away from home for a few weeks or months before the benefit kicks in. That’s because perks like this are meant to cover longer stays instead of short vacations. And like we talked about, you’re always covered at network rates when you have an emergency while traveling. Not all Medicare Advantage plans include a travel benefit. So if you’re like me and plan on traveling south every winter, you should look for a plan that offers one. Some are included in the price of your plan. Others are an option that you pay for only when you need it. Because every plan is different, contact your plan to learn more. Off exchange health insurance plans are purchased without going through the ACA exchange in your state. They can be purchased directly from an insurance company, or with the help of a broker. If you’re joining the ranks of workers 65+, Medicare might be the last thing on your mind. But when 65 is just around the corner, there are some important things you should know.
Four common Medicare questions 1. Can I delay signing up for Medicare Part B? If you have medical coverage through an employer, or you’re covered under your spouse’s employer plan, you can delay enrolling in Medicare Part B, which covers medical services, without paying a penalty. Many people don’t enroll in Medicare Part B until they stop working. Once you’re not covered under your employer plan (or your spouse’s), you’ll have eight months to enroll in Medicare Part B without paying a penalty. 2. How does enrolling in Medicare affect my HSA plan? If you have a health plan through your employer and it includes a health savings account (HSA), signing up for Medicare Part B, or being enrolled in Medicare Part A, will change things. You can stay on your employer plan, but you can’t add money to your HSA once you enroll in Medicare. If you’re considering this option, it’s a good idea to check with a financial adviser. They know the ins and outs of how Medicare will affect your HSA and your taxes, and can help you figure out your best option. 3. When should I start planning for retirement? Choosing a Medicare plan can be a long process! There’s a lot to consider and it takes time to find the right plan for you. If possible, I recommend starting your search about six to nine months before your retirement date. This gives you enough time to look into the plans that interest you. If you don’t have that much time, call plan advisers at private insurance companies that you’re interested in, or meet with someone who sells plans from multiple insurance companies (called a broker or agent) one-on-one. They can help you quickly find a plan that fits your needs and budget. 4. How will my current employer plan work with Medicare? If you have Medicare and also have health insurance through your job, these plans will work together. The coverage through your job will pay for some services, and your Medicare plan might cover some other services. If you have questions about off exchange health insurance plans, ask for advice from your current plan or benefits office. When I first started my career in the Medicare world, I was overwhelmed with all the new information I had to learn. I found that breaking it down into bite-sized pieces made it easier to understand. It took a lot of time (and patience), and one of the hardest parts was understanding all the different parts of Medicare. Here are some tips that helped me understand Medicare.
What is Medicare?Medicare is a federal health insurance program for people 65 and older, people under 65 with certain disabilities and people of all ages with end-stage renal disease. Medicare is partly funded by payroll taxes from most employers, employees and all people who are self-employed. The Medicare program offers basic coverage to help pay for things like doctor visits, hospital stays and surgeries. What are the parts of Medicare?Medicare is broken out into four parts.
Medicare Parts A and BParts A and B are known as Original Medicare. This is the most basic coverage you can get. Medicare Parts C and DParts C and D are available through private health plans. They’re both ways to enhance your health care coverage if you want more than what Original Medicare offers. Medicare Parts A, B, C and D explained:
When can I get Medicare? You’re eligible for Medicare when you turn 65. There are a few different times you can enroll throughout the year. These are known as enrollment periods. Check out the off exchange health insurance, or visit us for more information. October is National Ergonomics Month, and there’s no better time to evaluate your office environment. You may think that crafting an ergonomic workspace is mostly about getting certain chairs or keyboards, but in reality the principles of this field go far beyond comfort.
Making an office more ergonomic leads to healthier, more productive employees. Here’s how. What Is an Ergonomic Space?Ergonomics explores how people can work better and more efficiently. In general, an ergonomic workplace uses information about how people work to make changes that promote and protect employees’ health. This is critical for jobs with repetitive tasks like lifting, jobs involving many tools or jobs with long bouts of sitting and typing. When employees work in an environment that doesn’t make sense for them, they risk spending long periods of time in awkward positions or performing tasks that put them at a higher risk of developing musculoskeletal disorders (MSDs). And those injuries pose a big problem for the workforce. MSDs include injuries such as:
The Occupational Safety and Health Administration reports that 33% of worker illnesses and injury cases were due to MSDs. They’re also the leading cause of lost working days and reduced work. Ergonomics in the workplace may be even more important for aging Baby Boomers who are waiting longer to retire. For instance, sitting for long periods and with poor posture can lead to lower back pain. It’s a condition that affects all age groups, but people over 55 experience it more frequently. About 47% of workers older than 55 have arthritis, while 44% have hypertension, and they are the most likely age group to develop carpal tunnel syndrome. An office environment that doesn’t fit their needs can exacerbate these issues. How to Improve Ergonomics in the WorkplaceCreating an ergonomic environment starts with assessing your current situation. Consider the tasks your employees do in a typical day: Walk around desks, through a warehouse or along an assembly line to observe the repetitive movements employees perform. Note where you observe poor posture, strenuous lifting requirements or heavily used tools, and look for opportunities to make the employees more comfortable and less prone to injury. Make special note of any adjustments employees have made to their space or items themselves, such as placing cushions on desk chairs; they may indicate that your employees already know where there’s room for improvement. Once you have a list of possible hazards in hand, consider following the guide to implementing an ergonomics program in the workplace created by the Centers for Disease Control and Prevention. The guide recommends a hierarchy for making changes, starting with eliminating risks that could cause falls, slips or injuries. You can also change the way people work and ensure they have equipment that lessens MSDs, such as adjusting chairs and monitors to the appropriate height for good posture or introducing assisted devices for lifting and moving products through a warehouse. If you’d prefer having a professional make the assessment, ergonomics experts can come to your office to perform an analysis and make recommendations. However, just making a few small changes with your workforce’s needs in mind is enough to make a difference and keep your employees working in style — and, more importantly, in comfort. Do you want to know more details about health insurance please visit our service area. |
Author
Archives
January 2020
|